The vast majority of those who read the posts on this site show an interest because of problems with breastfeeding. I have pointed out many of those symptoms before: pain, poor weight gain, poor latch mechanics, reflux and so forth. As our awareness about tongue tie and lip tie increases, more moms will be sharing their stories. We often underestimate the power of sharing a Facebook status, liking a Facebook page, or tweeting out information.
Sometimes, parents will come across information on social media that piques their interest, even if they aren't experiencing a specific problem with breastfeeding. One of the more common ways that manifests itself is when they see a picture of a lip tie. I wrote previously about how upper lip ties (ULT) can affect breastfeeding. Pictures of thick or tight lip ties seem to pop up everywhere. Not uncommonly, parents will see these pictures and then take a peek under their own children's lips. Some are surprised to find what they think is a lip tie. Some will come to see me for treatment; others will email me for advice. Hopefully, this post will clarify some misunderstanding to avoid unnecessary concerns for those parents.
Those of us who frequently diagnose and treat ULT use a classification system to describe where the frenulum attaches. Class 1 lip ties are quite rare (it indicates little to no visible attachment). To date, I've seen more than 1500 babies and have yet to see a class 1 tie. A class 2 ULT will insert somewhere on the gumline (gingiva) above the edge of the gumline. A class 3 ULT will insert at the edge of the gumline, adjacent to a structure called the anterior papilla. Finally, a class 4 ULT will wrap around to the hard palate.
Class 2 Frenulum (no restriction noted - good flanging)
Class 3 Lip Tie (Central restriction noted)
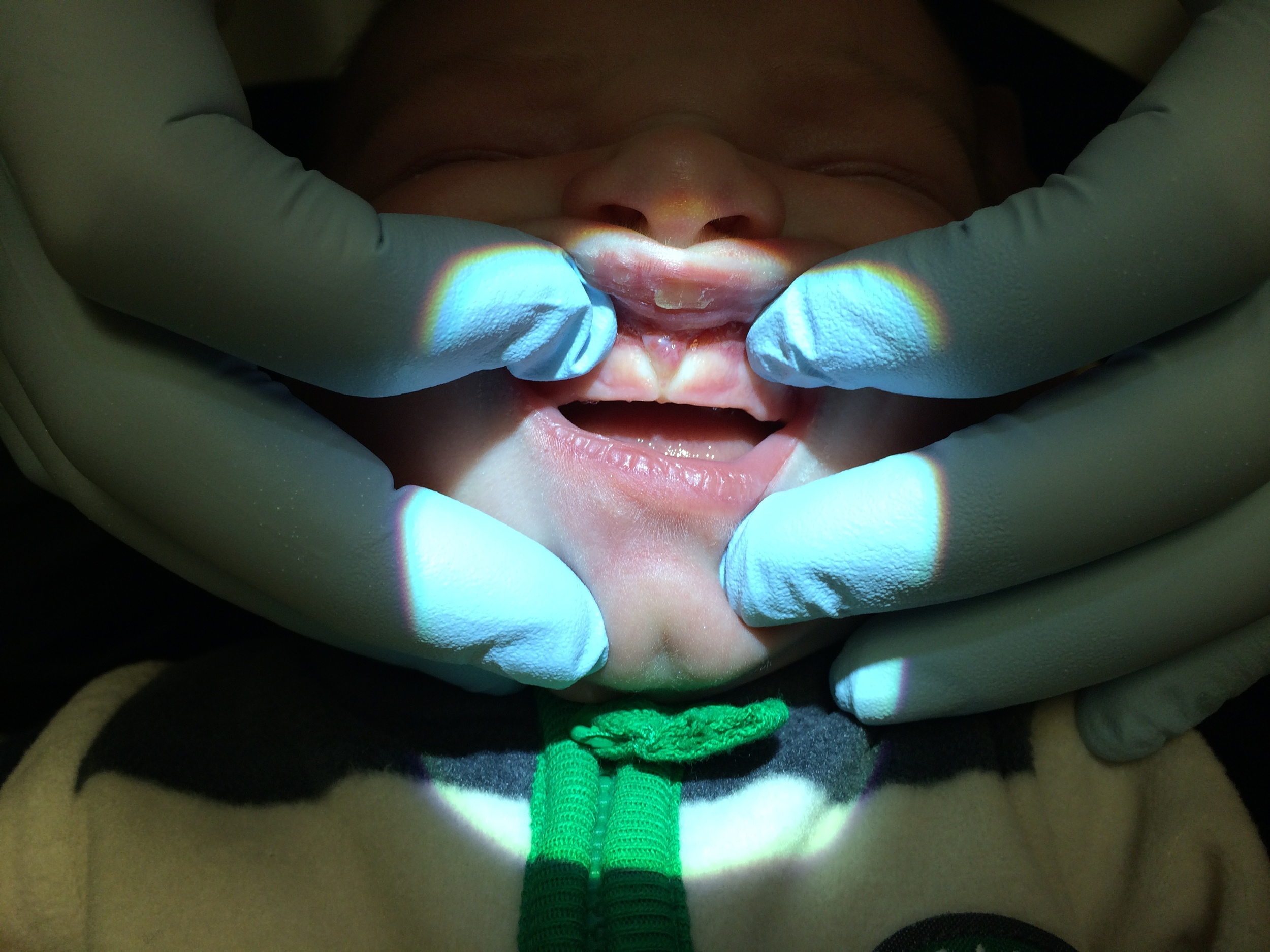
Class 4 Lip Tie (Central restriction noted, bone notching is present)
This classification system just describes anatomy. It does not determine severity, like a cancer staging classification does. A class 4 ULT isn't "worse" than a class 3 ULT - what matters is the degree of restriction. This degree of restriction can be determined by feeling the lip and trying to elevate it, mimicking the flanging motion needed on the breast. Alternatively, an IBCLC (international board certified lactation consultant) can evaluate what the lip is doing on the breast.
The most important thing to recognize, therefore, is that the classification used to describe the attachment of the labial frenulum to the gum can describe normal labial frenula as well. Many times, I will get an email asking for opinions on a baby's "class 3 lip tie" in situations where neither the baby nor the mom experiences breastfeeding problems. So in this instance, the baby has a class 3 frenulum.
To illustrate the distinction, we will examine an important study out of Sweden from 1994 by Flinck et al. This study examined 1021 newborns were studied over 8 months to record normal oral findings. Keep in mind that these babies weren't having particular problems - they were just being observed. Of those 1021 babies, only 68 (or 6.7%) had "buccal" insertions of the frenulum (this would indicate a class 1 or 2 attachment). 782 (76.7%) had class 3 attachments and 170 (16.7%) had class 4 attachments.
Keeping this in mind, I maintain that the location of the frenulum's attachment to the gumline CANNOT be a deciding factor on whether or not a frenulum is tied. If that were the case, the Flinck study would justify treatment in 93% of babies, and we know that number can't be right.
If restriction is noted, and the restriction is from the frenulum itself, then treatment is warranted. But in what other situations would treatment be plausible if breastfeeding weren't problematic? The two most common instances are dental decay and a central gap in the teeth (diastema).
The most important paper regarding the labial frenulum and premature dental decay comes from Dr. Larry Kotlow. In this study, he associates the presence of a prominent maxillary labial frenulum to premature dental decay of the two teeth on either side of the frenulum (the central and lateral maxillary incisors). The most likely mechanism of this premature decay is that a prominent frenulum can allow for pocketing of debris that cannot be cleared away, giving bacteria a reservoir of material to use. In my experience, the frenula that have a "hooding" appearance (like an awning over a patio) are the ones at highest risk. Because the majority of kids have class 3 or 4 frenula, but the majority of kids don't get this premature dental decay, I don't treat preemptively. I think that's bad medicine. But once decay is seen, treatment should be rendered.
The much more common question I get is about a central diastema or gap in the front teeth. Some parents are very worried about gap formation - they have brought otherwise asymptomatic babies to me before teeth have even come in, asking for revision. More commonly the gap is noticed once the front teeth come in. I still don't like to release those frenula at that stage - the gap can be temporary. As more teeth come in, the incisors can rotate forward, and the gap can be obliterated without the need for any intervention. My preference is to wait until all the teeth are in before deciding on a revision. Obviously, there are some exceptions - the severely thick frenulum or the ULT that is pulling on the gumline hard enough to cause notching of the border of the gumline will always have a gap, and treatment is reasonable. Other instances where treatment is helpful is when the child is experiencing pain from repeated minor trauma - this can occur during eating or brushing teeth. Regardless, it's important to understand that both a lip tie and an untied normal frenulum can cause a gap between the teeth. It's often more about the presence of tissue that can cause the gap, even if that tissue isn't under tension. Finally, it's important for parents to understand that releasing a frenulum that's causing a gap may not result in closure of that gap. Dental spacing is much more complex than the simple presence or absence of a low frenulum. If parents want a frenulum released to "prevent the need for braces", I advise them that there's no guarantee in the result because of the variable causes of abnormal spacing.
A normal frenulum can act as a space holder between teeth and cause a gap, like elevator doors that close on you. The mere presence of tissue (like the guy in the red shirt) can hold the teeth apart. A lip tie, which can also have abnormal bulk, has added tension to keep the teeth apart, just like someone using active force to keep elevator doors open. Both a nornal frenulum and a tie can cause a gap in those teeth.
While some may argue that this is an issue of semantics, I feel that it's an important distinction to make. When parents realize that what their child has is considered normal, it makes non-treatment a much less stressful choice. My goal is to make sure that we are releasing the appropriate frenula for the appropriate reasons.